Contents
What is it?
The chronic venous insufficiency , also known as varices or varicose veins are swollen veins because of an abnormal collection of blood due to weakness, often inherited in the walls and valves of the superficial veins. This causes the veins to widen and dilate, so that blood easily pools when a person stands for a long time.
“When the vein is dilated it does not fulfill its function. These are in charge of making the blood return to the heart and that implies that the flow has to go against gravity: from the foot to the heart ”, Andrés García León , director of the Angiology and Vascular Surgery Clinical Management Unit , explains to CuídatePlus deGar Virgen de Valme University Hospital (Seville) and member of the Andalusian Society of Angiology and Vascular Surgery . “The veins have valves that prevent the return of that blood flow to the foot and facilitate the rise.
However, if the vein is dilated, the valves do not fulfill their function and the flow is reversed, which causes the dilation to increase and problems such as edema, swelling of the leg or, in more advanced stages, ulcers or phlebitis ( thrombosis of a varicose vein) , among others “.
This pathology is much more frequent in women . The appearance of varicose veins is up to five times more frequent in them than in men. It usually occurs in the veins of the legs , however, it can also affect the esophagus, the anal region, the vulva or the testicles.
Causes
Among the main causes of the appearance of varicose veins, three stand out.
First, and if it is primary varicose veins, there are congenitally defective valves . The valves are responsible for circulating blood to the heart, so if they do not work properly the blood accumulates in the vein causing swelling.
The thrombophlebitis causes the same effect. In this case, they are thrombi, or what is the same, clots, which hinder circulation. This situation can occur, for example, after prolonged periods of bed rest.
The third most likely cause of varicose veins is pregnancy. Fortunately, varicose veins that appear during pregnancy are secondary and tend to disappear between two and three weeks after delivery.
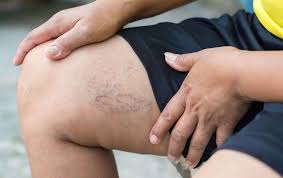
Symptoms
The most common clinical manifestations are:
Heaviness of legs.
Appearance of varicose veins with visible veins.
Edema.
Swelling.
Appearance of pain.
Cramps
Cushioning sensation.
In more advanced stages of the disease, venous ulcers, ocher dermatitis (darkening of the skin), or bleeding in complicated varicose veins may appear.
Prevention
Currently, there is no measure that helps prevent the appearance of varicose veins .
However, García León highlights that a healthy lifestyle; perform physical exercise; and avoiding overweight, obesity and sedentary lifestyle, contribute to the fact that, if a person is at risk of developing varicose veins, these are more controlled.
Types
There are different ways to classify varicose veins. The main one, at a medical level, is the CEAP ( Clinical-Etiological-Anatomical-Pathophysiological ) classification , which establishes a grading of varicose veins based on the clinical presentation, etiology, anatomy of the vein and the pathophysiology of it.
Diagnosis
The first recommendation that patients should follow in order for the diagnosis to be made is to go to a vascular surgery specialist. The expert is fully qualified to, only with the clinic and a physical examination, give a first diagnosis that is usually quite accurate.
Subsequently, the performance of a venous echo-Doppler usually provides more specific information on the anatomy of the varicose vein and on the therapeutic options that can be established.
Treatments
The pharmacological treatment of varicose veins is focused on alleviating the symptoms and preventing the disorder from getting worse. Some oral venotonic drugs are effective. The most used are Daflon ( diosmin ) , Venosmil ( hydrosmin ) and Venoruton (oxerutins), among others.

To alleviate symptoms, experts also recommend a series of measures:
Wear compression stockings. These garments mechanically help push blood from the capillaries to the heart, preventing stretching or injury. Despite the discomfort that they may cause, its use is especially indicated in the summer months, since with temperatures above 25 degrees there is a risk of worsening disorders associated with venous return.
Avoid exposure to the sun for long hours , lying down and not moving, and especially during the hours of maximum heat, which would lead to an intense and prolonged vasodilator effect.
Apply cold showers to the legs, making the jet impact in upward circles.
Avoid standing for a long time , especially in the case of people with a family history of the same type.
Use gels with a cold effect by gently massaging upward or with venotonic active ingredients.
Lie down and raise your legs above the height of your heart , after long periods of sitting or standing, and when sleeping.
Walk on the beach and bathe from time to time, as the fresh water activates circulation and improves the feeling of tired legs. In this case, it is necessary to shower after bathing to remove the salt, as it dries the skin, and apply moisturizer.
Avoid being overweight, obese and sedentary.
Do not wear clothing that is too tight .
Wear comfortable shoes, dispensing with high heels and flat shoes as much as possible.
Moisturize the skin daily.
Use sun protection all year round, as it helps reduce blood leakage.